The perception of time never ceases to amaze me. When I was undergoing chemo, the three-hour sessions felt like an eternity, and the first few days after my poisoning sessions dragged on while I was feeling sick. Then poof, just like that, 14 days had passed and, I was sitting in the chair getting my next infusion. During the first four weeks of radiation, the 40 minutes drive to and from the hospital felt was a great time to catch up on podcasts. Then last two weeks, I was counting every second my newly tanned insides were not near a bathroom for the inevitable code brown moments. Then I made it to the rest and recovery period, eight weeks straight with no medical appointments except for a quick lab visit to flush my port.
I was ecstatic to have eight straight weeks without doctors, scopes, poking, and prodding. During the first few days, I enjoyed time away from the doctors and nurses, but then it just felt strange. Transitioning from six months of doing something every day to kick cancers ass to recovery mode was harder than I thought, and time was crawling again. Now that I didn’t have to run somewhere every day, I finally had time to reflect on all the shit I had just gone through. We already knew the tumor was non-existent from the scans right after chemo, so this was reassuring. Still, there were 7 weeks of literally doing nothing ahead of me, and that is a lot of time to wonder where the future would take me.
- Will I need surgery?
- Did the lymph nodes shrink?
- Did radiation break something?
- They said not many people qualify for watch and wait, will I be that lucky?
- What if it comes back?
- Am I going to shit myself?
- Will my hands and feet ever stop tingling?
- And on, and on, and on…
Fortunately for me, during this period, I started a new job, so that took my mid off of things a bit and sped up the perception of time. Leave it to me to add in another stressful situation during the middle of fighting cancer, but hey, why not, right?
Two weeks after having my insides tanned by radiation and taking chemo, I was sitting on a plane headed for California to start a new job. In case you are wondering, I took Imodium before the flight, and I made it without any complications. I completed onboarding week and made it back home without pitching a deuce in my pants, so win, win. If you happen to be one of my new co-workers and stumbled upon this, you’re welcome. 😀
The new job kept my mind off the recovery period and ‘what-if” mental games, especially since I got to travel a bit and get out of the house where I just fought for my life for six months.
Even though my medical condition is protected federally as a disability, I was very transparent with my new employer. I wanted to make sure my new boss, and HR team, knew I needed time off for my upcoming scans and scopes. The last thing I wanted them to think is, “oh great, the new asshole is interviewing already” when in fact, this “asshole” was literally getting scanned and scoped. Anyway, the day for CTs and MRIs finally arrived.
Like the previous scans, these were fairly straightforward. I started off the day getting my port accessed so they could inject contrast for the CT and MRI scans. CT was up first. I applaud the mixologist on the contrast recipe, this one made me feel extra flushed and gave me the most realistic “I pissed myself” feeling yet. My overall Yelp review is a 9/10, would recommend and definitely will visit again. Then I was off to my own personal dubstep machine (MRI), which way more spacious than the last few. The took a series of scans without contrast, then they brought me out of the tube to up the difficulty factor a bit with some glucagon. They use this to slow down the intestines so they can get better images. I wasn’t sure if it was going to make me nauseous like last time since I was already nauseated from chemo. But it turns out the answer is yes, even when I’m feeling fine glucagon can turn on the purge reflex. Luckily I didn’t feel the need to redecorate the inside of the MRI machine thanks to some deep breathing. After a few more scans, they pumped in contrast, which I didn’t feel, and I was done.
Then the waiting game started, but it didn’t last very long as the radiologist and my oncologist released the CT results that evening.
1. No CT evidence for residual tumor (please also refer to same-day MRI pelvic exam). No suspicious lymph nodes or abnormalities in the mesorectal fat.
2. No evidence of metastatic disease in the chest, abdomen, or pelvis.
Lots of words to say, “the CT scans look good.” This was fantastic news, but after I read it, I maintained a cautious optimism since we had not seen the MRI results or the scope. As I saw it, there is no need to get excited when things could change in a heartbeat. The next morning I got a notification my MRI results were ready., so I wasted no time opening them up:
1. There has been a positive to treatment, with a corresponding tumor regression grade of mrTRG-1. No residual disease is appreciated.
2. No suspicious lymph nodes.
So now I had two scans telling me things “looked good,” but I continued my cautious optimism. I still hadn’t seen the scope results, anything could change. After waiting anxiously for a week, it was finally time to get scoped.
I never thought my wife and I would look forward to having a camera shoved up my nether regions, but this was the one and only time that would happen. I knew this scope session was going to be more uncomfortable than the previous ones, given how the troublesome the enema preps were. Apparently, frying your backside with radiation for six weeks can have some lasting effects.
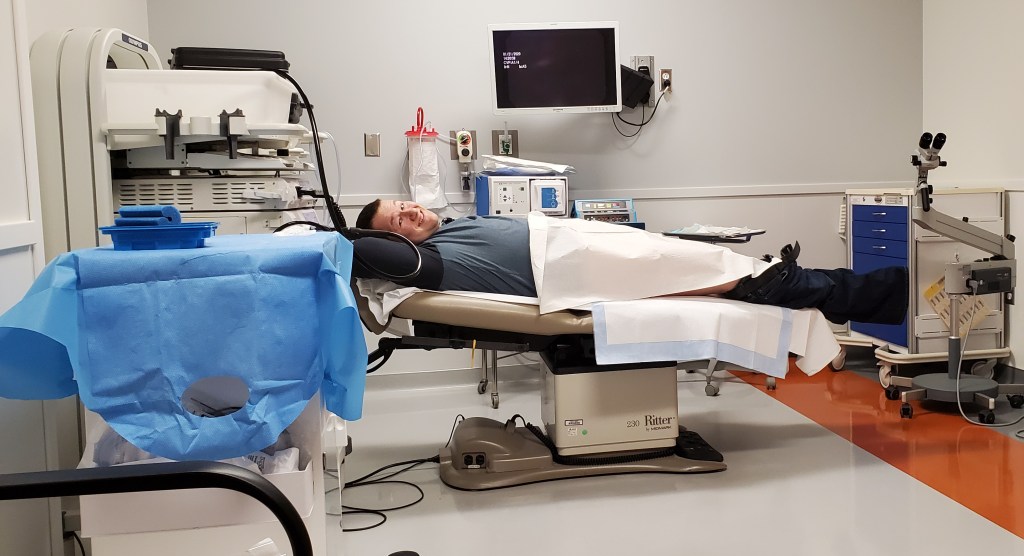
Assuming my position on the table, it was time for the moment of truth. After a few painful, cramping moments, I was able to relax enough to look at the screen. Where the tumor had been, continued to be tumor-free, and the surrounding area had not suffered any noticeable radiation damage. Then they needed to look up further to make sure no surprises hid around the bend in my colon. As they tried to make the turn, my stomach cramped horrifically, this is the point where I about crappie-flopped off the table. After what felt like 20 minutes, they made it around the corner, and things looked fine. Then they made their way back out with the camera, taking their time to ensure every inch was inspected. After they were done, I got cleaned up ASAP so we could get the final verdict.
Ass cancer Jesus informed me that based on the clean scans and the scope, I had what was considered a medically complete response to the treatment. Because of this, I was considered a candidate for the “watch and wait protocol.” However, before making my decision about further treatment, he needed to go over the pros and cons of both paths.
First, the cons of wait and watch. If I went with this approach, and the tumor returned, they would need to do the resection surgery at a later time. And since I waited, they could not ensure clean margins like I had now. This means they might not get everything during surgery; however, the likelihood of the tumor returning to the same location was very low. Now the pros. Electing to watch and wait, means I avoid a long list of complications from resection surgery, especially since there is no trace left of the disease.
Ok, now the cons of surgery if I elected that route. Several complications can occur from resection, including incontinence, leakage, permanent ostomy, etc. The list of pros was short but included having exceptionally clean margins given I had just had chemo and radiation.
As a final point of reference, of the 30 people who qualified for this protocol over the last 10 years, only 2 choose to have the surgery instead of waiting. Yeah, you read that right only 30 people in 10 years have even qualified for this protocol, that’s insane! One of the wait and watch patents had a regrowth, but it was successfully removed through surgery.
Now it was decision time, surgery, or no surgery? It should come as no surprise, I elected the quality of life option versus surgery. Especially since there is no trace of the tumor visible on any of the scans or scopes. Yes, it could come back, but it would likely show up in my liver or lungs rather than my rectum anyway. So, yeah… no thanks, please keep the scalpel away from my pooper!
One of the questions I had was about treatment options if a tumor did regrow. Since they will be aggressively monitoring the area, the first course of treatment would be surgery, followed by chemo if necessary. I asked them why they wouldn’t do radiation again, and I learned an exciting fact. I have received my lifetime maximum dose of radiation in my nether regions. So in the unfortunate event that something does re-appear in that area, radiation is off the table.
So, what do things look like from here on out? Lots and lots of scans and scopes for the foreseeable future. Here is my watch and wait protocol schedule:
- Flexible sigmoidoscopy
- Every 2 months for 6 months: Until 6/2020
- Every 3 months for 3 years: Until 11/2022
- Every 6 months for 5 years: Until 11/2024
- Every year for 10 years: Until 11/2029
- 3T MRI of pelvis
- Every 4 months for 2 years: Until 1/2022
- Every 6 months for 2 years: Until 1/2024
- Yearly for 2 years: Until 1/2026
- CT CAP
- Every year for 6-8 years: Until 1/2028
- Colonoscopy
- Annual
- CEA at every clinic or endoscopic visit
“Luckily,” I get to sleep through my next scope visit since I’m due for my colonoscopy. I’ll gladly deal with one day of blasting the toilet for colonoscopy prep if it means not having to be awake during the procedure. Especially since I look at the sigmoidoscopy schedule, and know that I’ll get a quarterly probing for the next three years.
Now that I’ve received the all-clear, you’d think I’d be on cloud nine. However, for some reason, I still find myself remaining cautiously optimistic. I’m not sure if its because I see 5+ years of scans and scopes, some form of PTSD, if it hasn’t sunk in yet or a combination of all the above. Despite all that, I am incredibly thankful for everyone that was there for me during this shitty time. I’m thrilled to be called a survivor that can share many more years with my wife, kids, family, and friends.
I know a lot of people are waiting for this post, so I will end here. I will have a follow-up post shortly to discuss some post-cancer celebrations I’ve had.

Congratulations on your good news, Ben!! Remaining a bit wary and not quite as celebratory as people would expect is how I felt as well, and I found that curious. Like you said, there has been a lot of trauma and still constant monitoring to come.
That being said, things sound great and I’m sure you and your family are very grateful. Best of luck!!
LikeLike
I am so glad you had positive results. I will continue to pray for you Ben. Congratulations on your new job. Go out and live life with a vengeance. God is good. We all have so much to be thankful for. So LIVE-LAUGH AND BE HAPPY!!!!!!
LikeLiked by 1 person
Thanks Ellen!
LikeLike
Oh Ben, I am so pleased with this outcome, you have such a level head on your shoulders, you are honest and truthful. As a nurse, I realize the future still holds a question mark for you, but what do any of us know about God’s plan for our life, our future with our family. After I did my mission trip to Haiti, I came back a changed women, our possessions are expendable, our life with our family is our joy and salvation, live every day to it’s fullest. I wish many years ahead for you and your family. This post is the best thing I have heard. Remain true to yourself, you are AMAZING!
Love, Melanie
LikeLiked by 1 person
Ben I can’t tell you how happy this post makes me! Your strength through all this is truly amazing. Stay strong.
LikeLiked by 1 person
Thanks Michael, I have a big hug saved up for you next time I see you!
LikeLike
Ben,
This is great news—a survivor indeed. You will be able to help so many others throughout your life having endured this trauma. As a family member, I am gratefully for your courage, the knowledge and skill of your treatment teams and most of all to God. Love you—Aunt Patty
LikeLiked by 1 person